Millions of people with chronic respiratory diseases such as asthma and COPD are among the most vulnerable to the corona pandemic. The best protection is offered by an optimally adjusted therapy of the inflamed lung areas – and this could receive an innovative boost through Nasal Long-Term Inhalation therapy (NLI therapy), which is currently being developed in Marburg.

First you might only feel a slight pull in the chest, but then tightness spread. Your breathing accelerates. Your heart beats faster. You begin to panic because of what’s happening, but the panic only makes the pain worse. Those who have known the threatening feelings that come with shortness of breath never want to experience them again, of course. But for many patients with chronic lung diseases, this is daily reality: They live with the fear of not getting air from one moment to the next.
The number of sufferers is significant: For example, common lung diseases such as asthma and COPD affect an estimated 15 million people in Germany alone. And their concerns are now increased for new reasons: These patients belong to the corona risk group, and they would experience an extremely serious medical condition in the event of coronavirus infection.
The Limits of Conventional Inhalation Therapy
In advanced disease stage, chronic respiratory patients require certain medicines. Their active ingredients – usually inhaled – lead to, among other things, a widening of the bronchi, which quickly provides air in an emergency and prevents further attacks of respiratory distress over the long term. The inhalation of these ingredients is intended to guarantee that the active substance being used reaches its destination quickly: the smallest branches of the lungs, in which respiratory diseases happen.
In reality, however, there are a number of hurdles in the way of this goal: the use of small inhalation systems (dosing aerosols), with which patients usually inhale the active substance two to three times a day, is extremely prone to errors. Complicating matters is the long distance that these tiny active particles have to travel from the mouth to the small lung branches. “What patients inhale of the drug and what ultimately arrives in the lungs is comparatively too little,” says Prof. Dr. Ulrich Koehler from the Department of Internal Medicine, Pulmonary Medicine and Sleep Medicine in Marburg. Also, if patients take several medications every day, they are bound to lose track or they forget to take them on symptom-free days.
All in all, inhalation therapy therefore places considerable demands not only on coordination abilities, but also on the continuous cooperation of the patients. The result can be a fluctuating dosage of the active substance, which can significantly jeopardize the success of the treatment.
The possibilities of nasal long-term inhalation
So how can inhalation therapy be optimized for the benefit of patients? In the search for opportunities for improvement, a group of researchers from the University of Marburg (Prof. U. Koehler), the Technical University of Middle Hessen (Prof. V. Gross and Prof. K. Sohrabi) and Thora Tech GmbH (Dr. Weissflog) have found a surprising answer: Following the current concept of Nasal Long-Term Inhalation (NLI), patients should continue to inhale via the nose in the future – and they should also do so in their sleep: “It’s about taking advantage of the night phase”, says Prof. Koehler.

According to the researchers’ theory, the sleep phase of patients offers the best conditions for the success of inhalation therapy. There are several reasons for this: On the one hand, there is sufficient time at night to administer – according to the principle of “long-time/low-dose” – using small amounts medication over a longer period of time. This method could help reduce side effects and also relieve patients who need to inhale their medications several times during the day. On the other hand, symptoms are often particularly pronounced at night and in the early morning, when the airways become narrow and mucus has accumulated more in the lungs. Against this background, it is possible to directly counteract this discomfort by taking the medication at night.
How nighttime inhalation works through the nose
However, another question will be decisive for the success of the therapy: Will the researchers be able to dose the active substance better using the new method or deposit it in the target area of the small airways? The solution to this problem lies in the combination of inhalation with an already established therapy. The new method is primarily intended for patients with severe COPD. These patients are already supplied with oxygen and especially with night-time ventilation (BIPAP = biphasic positive airway pressure).
BIPAP is an already established ventilation therapy that supports patients in breathing. With the help of a machine-generated overpressure, the airways are opened, and the respiratory muscles are relieved. Prof Koehler sums up the special feature of Nasal Long-Term Inhalation: “We combine the congestion pressure method with inhalation therapy. With pressure, the airways are shaved, and then the drug is applied using a nebulizer system. This combination brings us much deeper into the periphery of the lungs than we have achieved so far. With congestion pressure, the way over the nose is ideal.”
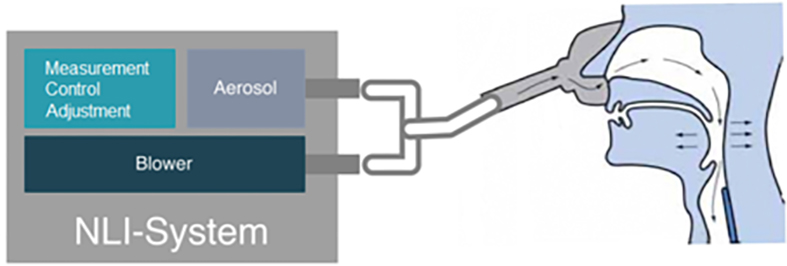
Effectiveness must be evident in patients’ everyday lives
This ambitious research project has now reached a crucial point: Further studies will further demonstrate the effectiveness of nasal long-term inhalation. And it is not only bronchial-enhancing active ingredients that can be administered via nasal inhalation. Cortisone, antibiotics and the moist inhalation of brine can also be applied in this way.
Nasal Long-Term Inhalation therapy, therefore, has great potential for intelligent and automatically controlled medication, which could take patient care to a new and better level. The question of patient adherence to therapy – so-called compliance – is now increasingly coming to the fore: Do patients accept the novel therapy in their daily lives and thus improve compliance? What Prof. Koehler knows ist that “a therapy like NLI can only be successful if patients are convinced that it helps them.”
If this succeeds, Nasal Long-Term Inhalation could soon find its way into patients’ everyday lives – and the idea of healthy sleep could become even more important for those affected.
Also interesting:
> Sleep apnea: how poor sleep causes health risks
> Particle Therapy: Fighting Cancer gently

