Germany’s lack of rural doctors also affects us here in Hessen’s mid-central region. The Lahn-Dill rural physician network breaks new ground to ensure medical care by general practitioners in the district. The network’s commercial head, Lars Bongartz, reports on the challenges in setting up the network and the necessary building blocks for referring patients to doctors and practices.

Commercial head of the Landarztnetz Lahn-Dill GmbH
Being a rural physician used to be almost a romantic, worthwhile goal for many doctors; today, however, it no longer attracts many medical graduates. Instead, young people are drawn to urban areas and large cities. We must find a solution to this problem.
Our experience shows that once young doctors experience first-hand what it’s like to be a rural physician, most of them stay in these communities. We want to make such initial contact with the profession of rural medicine possible – “we” are the Rural Physician Network (in German, “Landarztnetz,” or LAN). Our goal is to help protect general practioner patient care in rural Lahn-Dill areas. In the past five years, we’ve built a network that enables us to find successors for rural practices in our district -since many doctors in rural regions have no luck in finding a successor on their own.
Demographic change is everywhere
Demographic data told us years ago that medical care in rural areas would become scarce. That’s why we founded our initiative. So we asked ourselves: What needs to happen?
For some time now, there has been an increasing trend for physicians to take on salaried positions instead of running their own practice on a freelance basis. In the past, roughly 20 to 30 years ago, the salaries of freelance physicians were much better than in hospitals. Today, salaries in the inpatient sector are just as good. In addition, physicians in hospitals and clinics are more flexible and can change their place of work more easily if they wish. That’s why many doctors today prefer to work as salaried employees. Today, most medical school graduates have salaried positions in healthcare facilities.
In the private-practice sector, this possibility has only existed since 2004, when legal requirements for medical care centers were established. Since then, more doctors have been choosing this path. With the rural physician network, we have created a possibility for doctors to be employed with us in a rural medical practice.

Advantages for senior physicians
Traditionally, rural physicians sell their practices. Today, this opportunity arises less often because they can’t find a successor. This means many doctors have to close or give away their practices, which most doctors don’t want to do. Several reasons exist for this. Since most doctors also live in the area where they practice, they assume that their patients will continue to ask them for medical advice although they no longer have a practice. Another reason why physicians don’t like to close their practices is that they want to preserve their life’s work. With a suitable successor, they could satisfy both wishes.
And this is where we come in. We integrate private practices in the rural physician network. The network assumes the tangible assets of the practice, including the leasing contracts and employees. However, this is only on the condition that the physician continues to practice for 12 months. We need this time to find a potential successor, and the senior doctor has time to familiarize the new rural physician with his or her work and patients.
From the annual report of the medical statistics of the German Medical Association of 31.12.2018
In 2018, 392,400 doctors were practicing in Germany. Of these, 117,500 identified themselves as independent in private practice, while 39,800 identified themselves as staff doctors within medical systems. A quarter of the total practicing doctors plan to retire within the next 5 years. Their retirement will also affect numerous rural practices. According to projections by the German Council of Economic Experts (“Sachverständigenrat zur Begutachtung der Entwicklung im Gesundheitswesen”), there will be a shortage of 30,000 general practitioners across Germany in the next 10 to 15 years.
Opening professional doors for young doctors
When young doctors join us and are hired by a practice, they have three possibilities: If they realize that being a rural doctor is not for them, they are free to move on. If they like the profession, they can either remain employed indefinitely by the practice, or they can take over the practice and start it again as an independent private practice outside of the network. So we offer employee status with the option of private practice.
And these are not the only advantages for young doctors. In addition, the network offers them various employment models – they can work full-time or part-time and have a company car. From my own experience, I can say that once young doctors have settled in, they usually don’t find the rural physician existence all that bad – and they stay. In this sense, we are an important regional political project as well. The network improves medical care in rural areas by keeping practices open and by creating jobs. We currently employ 50 people at our sites – ten doctors and 40 medical assistants in different practices.
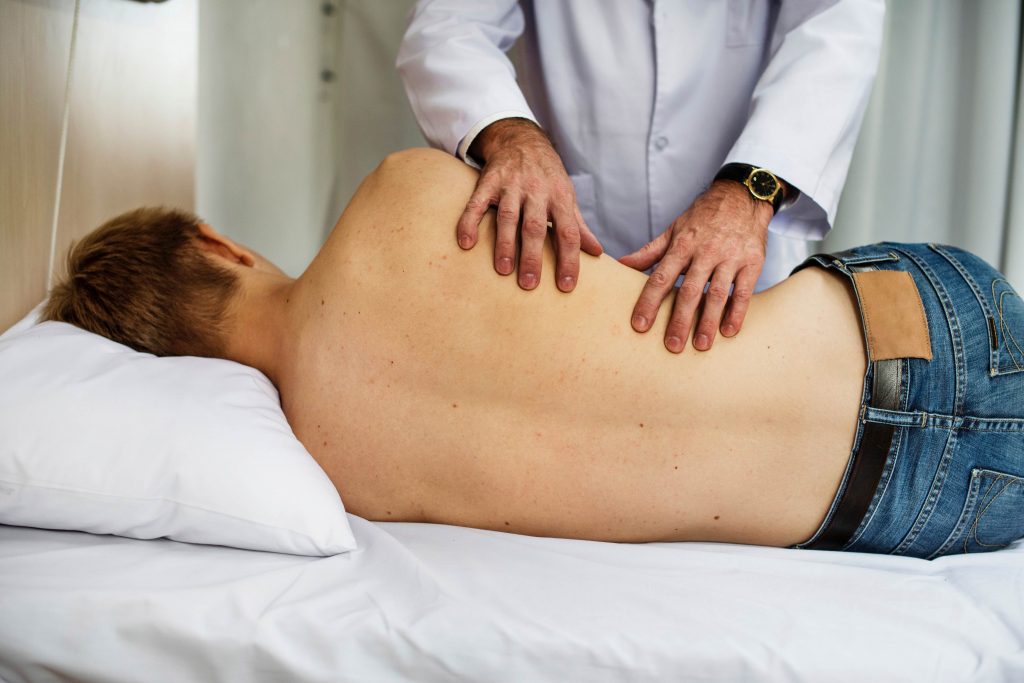
The rural physician network offers opportunities for the future
Unfortunately, the rural physician network owes its existence to several coincidences. In the future, it will not be able to exist the way it does now. We must take the next step to develop it further. One possibility would be to allow non-physicians – such as the medical assistants in the practice – to work as substitutes and not merely in delegation as is common until now. Plans have been made in this direction, but this is not yet legally possible. Another possibility is having a better regional management. This means there has to be patient transport systems that can take patients to physicians who are farther away.
The third possibility is further development of telemedicine. Until now, there have only been tests – for example, a digital consultation via video chat. But I think that will change sooner or later. People in rural areas will have to accept that their medical care will change in the future and that they will have to travel longer distances. They will also have to get used to digitalization in medicine – which is not negative in itself, but still unfamiliar to most people.
This change is coming, and it must come. However, through the rural physician network, we have created an opportunity to make the change as smooth as possible – and above all, to help shape it.
company profile
Landarztnetz Lahn-Dill
The partners of the rural physician network are Lahn-Dill-Kliniken GmbH and former first vice president of the physician network Lahn-Dill (A.N.R. e.V.), Dr. Michael Saar, from Breitscheid. The Lahn-Dill rural physician network – and its base at the medical care center in Breitscheid – were approved on April 1, 2014, by the admission committee of the Association of Statutory Health Insurance Physicians, Hessen.

